- Calcium & Bone Metabolism
- Update on Preoperative Parathyroid Localization in Primary Hyperparathyroidism
-
Hye-Sun Park, Namki Hong, Jong Ju Jeong, Mijin Yun, Yumie Rhee
-
Endocrinol Metab. 2022;37(5):744-755. Published online October 25, 2022
-
DOI: https://doi.org/10.3803/EnM.2022.1589
-
-
4,093
View
-
357
Download
-
4
Web of Science
-
6
Crossref
-
 Abstract Abstract
 PDF PDF PubReader PubReader  ePub ePub
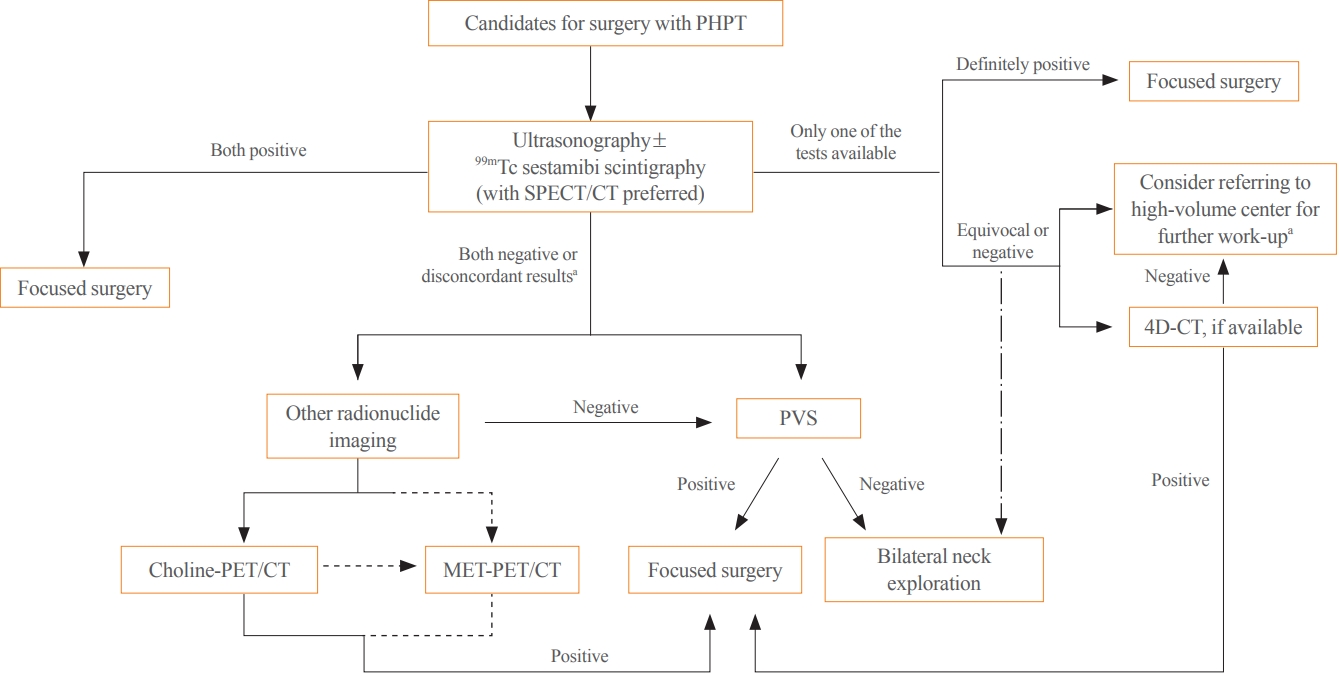
- Parathyroidectomy is the treatment of choice for primary hyperparathyroidism when the clinical criteria are met. Although bilateral neck exploration is traditionally the standard method for surgery, minimally invasive parathyroidectomy (MIP), or focused parathyroidectomy, has been widely accepted with comparable curative outcomes. For successful MIP, accurate preoperative localization of parathyroid lesions is essential. However, no consensus exists on the optimal approach for localization. Currently, ultrasonography and technetium-99m-sestamibi–single photon emission computed tomography/computed tomography are widely accepted in most cases. However, exact localization cannot always be achieved, especially in cases with multiglandular disease, ectopic glands, recurrent disease, and normocalcemic primary hyperparathyroidism. Therefore, new modalities for preoperative localization have been developed and evaluated. Positron emission tomography/computed tomography and parathyroid venous sampling have demonstrated improvements in sensitivity and accuracy. Both anatomical and functional information can be obtained by combining these methods. As each approach has its advantages and disadvantages, the localization study should be deliberately chosen based on each patient’s clinical profile, costs, radiation exposure, and the availability of experienced experts. In this review, we summarize various methods for the localization of hyperfunctioning parathyroid tissues in primary hyperparathyroidism.
-
Citations
Citations to this article as recorded by  - Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue
Anne L. Worth, Mesrop Ayrapetyan, Susan J. Maygarden, Zibo Li, Zhanhong Wu, Chris B. Agala, Lawrence T. Kim
Journal of Surgical Research.2024; 293: 618. CrossRef - Use of [18F]fluorocholine PET/CT in the detection of primary hyperparathyroidism in paediatrics: a case report
Helena Martínez Sánchez, Francisca Moreno Macián, Sara León Cariñena, Carmen de Mingo Alemany, Lidia Blasco González, Raquel Sánchez Vañó
Journal of Pediatric Endocrinology and Metabolism.2024;[Epub] CrossRef - A Rare Case of Hyperfunctioning Lipoadenoma Presenting as a Cystic Pararthyroid Lesion
Jinyoung Kim, Ohjoon Kwon, Tae-Jung Kim, So Lyung Jung, Eun Ji Han, Ki-Ho Song
Journal of Bone Metabolism.2023; 30(2): 201. CrossRef - Role of 18F-Fluorocholine Positron Emission Tomography (PET)/Computed Tomography (CT) in Diagnosis of Elusive Parathyroid Adenoma
Janan R Badier, Pokhraj P Suthar, Jagadeesh S Singh, Miral D Jhaveri
Cureus.2023;[Epub] CrossRef - Pitfalls of DualTracer 99m-Technetium (Tc) Pertechnetate and Sestamibi Scintigraphy before Parathyroidectomy: Between Primary-Hyperparathyroidism-Associated Parathyroid Tumour and Ectopic Thyroid Tissue
Mara Carsote, Mihaela Stanciu, Florina Ligia Popa, Oana-Claudia Sima, Eugenia Petrova, Anca-Pati Cucu, Claudiu Nistor
Medicina.2023; 60(1): 15. CrossRef - Diagnostic Performance of Magnetic Resonance Imaging for Parathyroid Localization of Primary Hyperparathyroidism: A Systematic Review
Max H. M. C. Scheepers, Zaid Al-Difaie, Lloyd Brandts, Andrea Peeters, Bjorn Winkens, Mahdi Al-Taher, Sanne M. E. Engelen, Tim Lubbers, Bas Havekes, Nicole D. Bouvy, Alida A. Postma
Diagnostics.2023; 14(1): 25. CrossRef
- Non-functional Pituitary Adenoma Detected on (18)F-fluorodeoxyglucose Positron Emission Tomography ((18)F-FDG-PET) in a Patient with Mucosa-associated Lymphoid Tissue Lymphoma.
-
Jin Ha Lee, Seung Jin Han, Se Eun Park, Mi Ae Cho, June Won Cheong, Mijin Yun, Yumie Rhee, Eun Jig Lee, Sung Kil Lim
-
J Korean Endocr Soc. 2008;23(2):137-141. Published online April 1, 2008
-
DOI: https://doi.org/10.3803/jkes.2008.23.2.137
-
-
1,826
View
-
19
Download
-
1
Crossref
-
 Abstract Abstract
 PDF PDF
- Magnetic resonance imaging (MRI) is the modality of choice for the detection and characterization of a pituitary adenoma. Uptake of (18)F-fluorodeoxyglucose (FDG) by intrasellar tumors, including pituitary adenomas, has been reported in several previous studies. We report a case where a pituitary adenoma was detected on FDG-positron emission tomography (PET), but the tumor was not detected with the use of sellar MRI. A 31-year-old woman was referred to the clinic due to a focal increase of FDG uptake at the pituitary fossa seen on whole body FDG-PET. The patient was receiving chemotherapy due to a recurred B-cell lymphoma of the mucosa-associated lymphoid tissue type. Subsequently, sellar MRI was performed, and images showed a small non-enhancing heterogenous cystic lesion in the midline of the pituitary gland, radiologically suggestive of a Rathke's cleft cyst. However, sellar MRI failed to identify a lesion consistent with a pituitary tumor that corresponded to the site of increased FDG uptake detected by the use of PET, despite the inclusion of a dynamic contrast enhanced sequence. Despite the negative findings of the MRI examination, basal and stimulated levels of the GnRH free alpha-subunit were profoundly increased. Therefore, we suspected the presence of a non-functional pituitary tumor in addition to a Rathke's cleft cyst, rather than pituitary involvement of a lymphoma, based on the hormone levels and PET scan findings.
-
Citations
Citations to this article as recorded by  - Clinical Characteristics of 16 Patients with Pituitary Tumor Incidentally Detected by18F-Fluorodeoxyglucose PET-CT (18F-FDG PET-CT)
Hyung Jin Kim, Gi Jeong Cheon, A Ra Cho, Chang Hoon Lee, Sang Min Youn, Se jin Ahn, Sang Eon Jang, Jung Min Kim, Yun Yong Lee, Ka Hee Yi
Endocrinology and Metabolism.2010; 25(4): 321. CrossRef
|